Malocclusion & Treatments
Not Only Diagnose, But Also Holistically Treat Symptoms!
Bite or occlusion refers to the way the upper (maxillary) and lower (mandibular) teeth & jaw are aligned with each other. Ideally, your teeth should fit easily within your mouth without any crowding or issues. Also, none of your teeth should be rotated or twisted. The maxillary teeth should slightly overlap the mandibular teeth so that the pointed ridges of your molars fit into the groves of the opposite molar.
Deviation from ideal occlusion is known as malocclusion (bad bite), which causes “bite disorder”. The temporomandibular joint (TMJ) becomes secondarily malaligned from a bad bite. Malocclusions are one of the major oral health problems ranking third after dental caries and periodontal disease. If not treated, it can affect one’s oral and digestive health, which will ultimately affect overall health.

Early Detection of Malocclusion
As a certified holistic and biological dentist, Dr. Maryam Horiyat could help adults and children to correct the way their teeth and jawline up. She uses several advanced tools and techniques to move teeth and sometimes the jaw into the right position.
Dr. Horiyat follows Dr. Weston A. Price’s theories and focuses not only on diagnosing and treating the symptoms of malocclusion but also on preventing the condition and its severity, thus, she strongly recommends the early detection and treatment of malocclusion for your children as early as seven (7) years old to correct and guide the growth of your child’s jaw to help permanent teeth come out straight, regulate the width of the upper and lower arches to optimize airway, create more space for crowded teeth.
By implementing more minimally invasive approaches, Dr. Horiyat believes that early detection not only helps to diagnose and correct teeth and jaw problems sooner without going through invasive jaw surgery but also may help cut down on the length and severity of the non-surgical treatments.
What is Bite Disorder or Malocclusion?
Malocclusion, also known as “Traumatic Occlusion”, simply means having a “Poor Bite”. When patients get headaches, clicking & popping jaw joints, age prematurely, or grind their teeth at night they have a bite disorder.
A bite disorder relates to the position of the lower jaw in relation to the upper jaw and to both TMJ joints. When a person brings their jaws together to chew or bite, the way the occlusal surface (chewing surface of the teeth) comes together can affect more than just those teeth. the force from the functional contact can affect other teeth, the gum, jaw muscles, jaw joint, the neck, and even the head. Patients who clench or grind their teeth may also exert force which could cause a breakdown of the oral structures and overall health.
causes of maloclusions
The major cause of maloccusion is inadequete nutrition in one’s formative years, as Dr. Weston A. Price so incontrovertibly prove in the early twentieht century. He indicated that malnutrient and the ensuing dental malocclusions result from inadequate maternal nutriction before and during pregnancy as well as during brestfeeding.

What Causes Malocclusion?
There are many reasons for malocclusion; however, any malocclusion needs to be treated. Some of the reasons are:
- The Difference in Size of the Lower & Upper Jaw
- Tooth Loss
- Obstructed Airway
- Impacted Tooth
- Cleft Lip & Palate
- Extended Bottle Feeding, Thumb Sucking, & Pacifier
- Irregular Shaped Teeth
- Hereditary
Conditions Causing Malocclusion
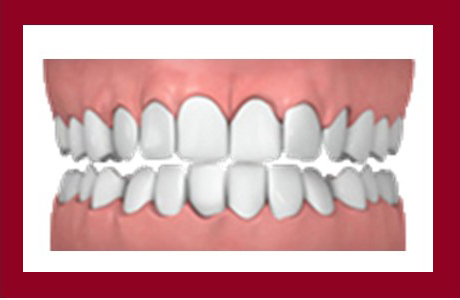
Overly Crowded
Crowded teeth can be difficult to clean properly. Lack of proper oral care can promote tooth decay and cause a higher risk of gum disease, and ultimately tooth loss.
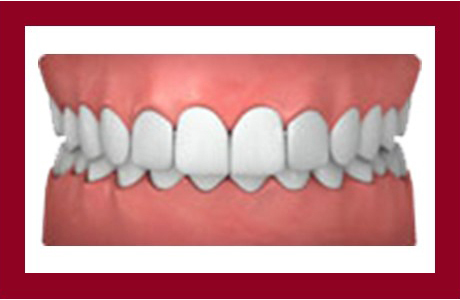
Overbite
When the upper front teeth are biting down right into gums, an increased overbite is caused when the lower front teeth can also bite into the roof of the mouth.
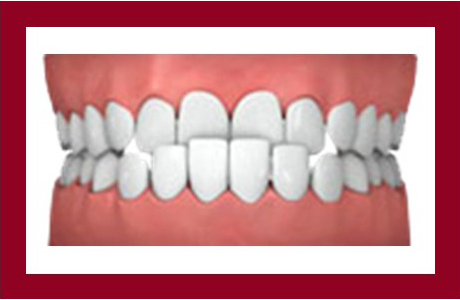
Underbite
Also known as anterior crossbite, underbite occurs when the bottom teeth protrude beyond the upper teeth and can interfere with the normal function of front teeth and molars and can lead to jaw problems.
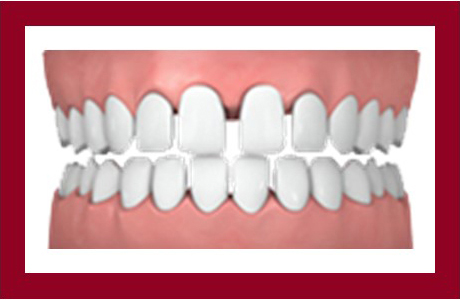
spacing
When there is too much or too little space for the teeth, it results in crowding which can adversely impact the eruption of permanent teeth. Gaps can cause teeth to shift into empty spaces and become loose.
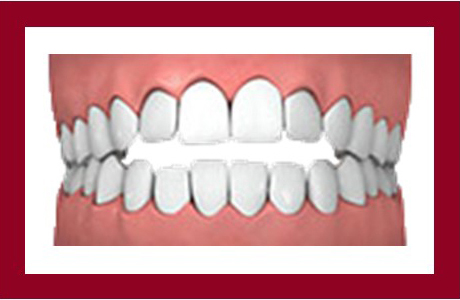
Open Bite
When the upper and lower front teeth do not overlap each other, it results in the formation of an opening of the mouth. This can also happen on the side of the mouth. An open bite can interfere with chewing and cause speech impairment and jaw problems.
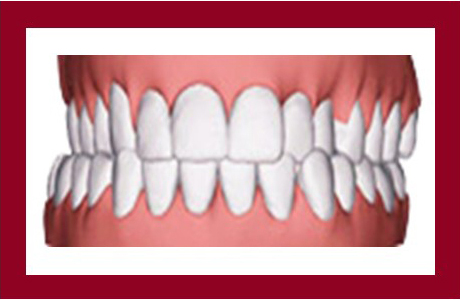
Crossbite
A crossbite can happen on either or both sides of the jaw when the upper front teeth are biting right inside the lower teeth. This condition can also affect your front or back teeth.
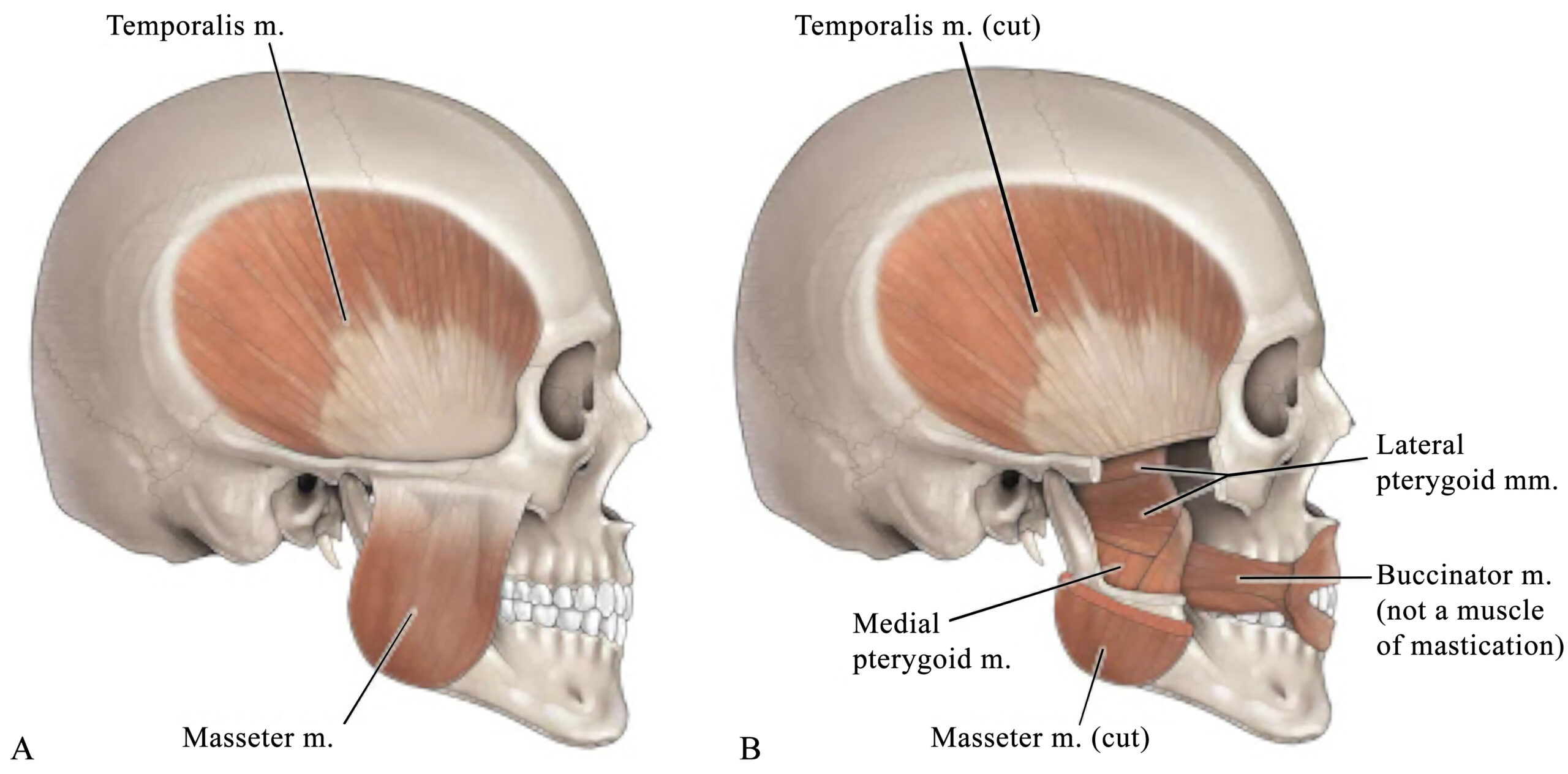
4 Main Muscles Involved in Bite Occlusion
The primary and accessory muscles of mastication work in a coordinated fashion to produce mandibular movement during chewing, talking, and yawning.
a big fan-shaped muscle that sits in the temporal fossa and inserts onto the coronoid process of the mandibular.
sits over the ramus and angle of the mandibular and acts to elevate the mandible.
attaches to the lateral surface of the lateral pterygoid and provides side-to-side movement of the jaw and protects the jaw.
attaches to the medial surface of the lateral pterygoid provides side to side movement of the jaw and elevates the jaw.
Types of Malocclusions
These muscles work together to generate incredible forces when chewing, grinding, or clenching. When the teeth are misaligned, the force can be destructive to the ligaments and bone which holds the teeth in place.
Class I Malocclusion
Class I Malocclusion is the most common type wherein the molar position and ability to bite are normal, but other teeth are misaligned in some way. These abnormalities can include overlapping or overcrowded teeth, rotated teeth, gaps between teeth, asymmetry, and open bites.
Class II Malocclusion
Class II malocclusion is diagnosed when a severe overbite is present. This condition, also known as retrognathism (or retrognathia), involves severe overlapping of the upper teeth and jaw over the lower jaw and teeth. The lower anterior incisors are positioned considerably behind the upper anterior incisors as the patient bites down.
Class III Malocclusion
Class III malocclusion is diagnosed when there is a severe underbite or crossbite. This condition, also known as prognathism, takes place when the lower jaw is larger than the upper, causing teeth of the lower jaw to be more visible. The lower anterior incisors are positioned edge to edge with the anterior incisors.
Malocclusion Symptoms
People experiencing any malocclusion or an imperfect positioning of the teeth when the jaw is closed, might not be aware that there is a problem. Depending on the classification of malocclusion, the symptoms of the disorder may be subtle or severe. Typical symptoms of malocclusion include:
- Tooth breakage & Tooth Loss
- Teeth Sensitivity & Excessive Wear & Tear
- Joint Noises or Pain in the Neck & Jaw
- Uneven Bite
- Improper Alignment of the Teeth
- Alteration in Face Appearance
- Discomfort When Chewing or Biting
- Speech Problems
- Mouth Breather
- Facial Collapse & Collapsed Bite
- Snoring & Insomnia
- Teeth Grinding (Bruxism)
How to Diagnose MALOCCLUSION?
Dr. Horiyat usually checks for malocclusion during their regular dental visits by performing the following steps:
- Ask questions about your past health
- Check the mouth & teeth
- Take digital radiography, panoramic Imaging, intra-oral camera, and i-tero element scanning
- Digitally capturing, measuring, and analyzing your complete bite (occlusal) story using hi-tech Tekscan
How to treat Malocclusion?
Some people with mild occlusion may not require any treatment, but everyone needs to be evaluated by a dentist.
There are two major pathways of treatment for malocclusion: Conventional Orthodontic Care & Functional Orthodontic Care. With conventional orthodontic care, the “cure” can often be worse than the disease. It consists of the extraction of four or more healthy teeth -typically bicuspids – followed by the placement of braces and retainers to alleviate crowding which is originally caused by the underdevelopment of the jawbone from improper diet during infancy and childhood. In contrast, functional orthodontics care uses guided growth and development of oral appliances or splints to encourage the growth of underdeveloped dental arches which will allow teeth and bones to grow approximately to their original genetic blueprint of development.
As an accredited holistic dental practitioner, Dr. Maryam Horiyat understands the root cause of malocclusions, their relation with inadequate nutrients, and the serious consequences of dental arch deformities. Dr. Horiyat has a deep appreciation for the pioneering functional orthodontic care of Dr. Weston A. Price. She follows in Dr. Price’s footsteps by offering functional expansion appliances such as Vivos System Guided Growth and Development Appliances.
Some children may need an early treatment called growth modification. For this, the child wears a device that helps move the jaw into a better position. This treatment works best during a child’s growth spurts and can be followed by braces.
Depending on your type of malocclusion and oral structure, Dr. Horiyat may recommend various treatments for patients of different ages. In some cases, all of these treatments are required to correct the alignment of different teeth and completely cure traumatic occlusion. These can include:
- Vivos Biomimetic Appliance Therapy
- Guided Growth & Development Oral Appliances
- Invisalign
- Removable Devices Like Retainer
- Braces
Looking Beyond Straight Teeth... Bite Correction Solutions
Vivos DNA Appliances
KOIS Deprogrammers
Invisalign®
Full-Mouth Rehabilitation
Replacing Missing Teeth
Dental Orthotics
SAY GOODBYE TO CROOKED TEETH &
Feel Better Look Better Live Healthier Smile & Shine for Life!
Schedule an Appointment with Top Certified Dentist in Orthodontics
Maryam Horiyat
DDS, AIAOMT . IABDM
Stars from over Reviews