According to the center for disease control and prevention, periodontal disease is one of the most common dental conditions experienced by millions of Americans. Treating this dental disorder can prevent future dental problems, but it also lessens the risk of overall health conditions attributed to gum disease. Studies demonstrate that you can prevent and treat such diseases once they develop. Your teeth can remain healthy and happy for life with the help of advanced periodontal treatments.
Periodontal Diseases
Periodontal diseases are the specific conditions that affect the supporting connective tissue around your teeth, better known as gingiva or the gums, and alveolar bone anchoring your teeth in the jaws. These diseases are among the most common chronic disorders.
Some common symptoms of periodontal disease include loose teeth, persistent bad breath or bad taste, red, swollen, or bleeding gums (can be spontaneous), and gums that have pulled away from your teeth.
Periodontal diseases have been plaguing humans for centuries. Some descriptions of periodontal structures and different ways of treating them were found in ancient writings of Egyptian and Chinese scholars. Today, periodontal disease has gained greater importance as the most common cause of tooth loss. In the past two decades, remarkable advancements have been made regarding the cause of these diseases, their diagnosis and pathogenesis, and appropriate therapies and treatment. Several terms are used interchangeably to describe the structures that make up the periodontium. Your tooth is suspended in the alveolar socket by collagen fibers. These collagen fibers, known as the periodontal ligament, are embedded in both alveolar bone and the cementum, which covers the outer surface of the tooth root. The periodontal ligament, the tooth root, and the alveolar bone socket collectively make up the periodontium. Overlying these supporting structures are the gingiva (the gums) and the alveolar mucosa. The periodontal disease indicates the involvement of the gingiva, the underlying attachment structures, or both.
Periodontal diseases either solely affect the gingiva, or are associated with the destruction of the underlying structures of the periodontium. The gingival disease most often indicates gingivitis, which is clinically recognized by redness, swelling, a change in the gingival margin position, and bleeding of the gums while brushing your teeth.
A very painful form of gingivitis is acute necrotizing ulcerative gingivitis, sometimes called trench mouth or Vincent’s infection. This disorder often occurs in adolescents and is marked by sudden onset, pain, and tissue necrosis.
The other type of gingival disease involves a manifestation of systemic disorders or hormonal disturbances. Acute herpetic gingivostomatitis is a painful representation of primary herpes virus infection.
Some health conditions such as blood dyscrasias, autoimmune diseases, and metabolic diseases can be associated with gingival inflammation. Other factors like pregnancy and puberty may also be associated with an increased incidence of gingivitis.
Specific medications could also contribute to the onset of various gingival diseases, such as hyperplasia and the enlargement of the gingiva.
Although gingival diseases are widespread, they are not considered as problematic as the periodontal diseases that destroy the underlying structures of the periodontium.
Periodontitis is one such disease; it develops when the inflammatory process of gingivitis extends into the periodontal ligament and alveolar bone, destroying both. As the periodontal ligament is demolished and the alveolar bone is resorbed, the epithelium of the gingiva pulls away from the root surface, causing periodontal pockets to form between gums and teeth. When left untreated, periodontitis will advance quickly, leading to loss of connective tissue, alveolar bone resorption, and formation of periodontal pockets.
More severe forms of the disease cause a loosening and, finally, the loss of teeth. While many of your teeth may lose their attachment structures, others may remain unaffected.
Adult periodontitis is the leading cause of tooth loss and the most frequently experienced form of periodontitis that appears in the third decade of life. Early diagnosis and proper treatment of adult periodontitis are among the most significant challenges of modern dentistry.
Other forms of periodontitis are primarily defined based on the age group they target:
- Generalized and localized juvenile periodontitis occur around the time of puberty.
- Prepubertal periodontitis, which is rare but quite aggressive, starts after the eruption of the primary teeth.
There have been reports of patients experiencing unique forms of gingivitis and periodontitis. Mild gingivitis may progress to advanced periodontitis, followed by tooth loss in just a few months.
Clinical Analysis
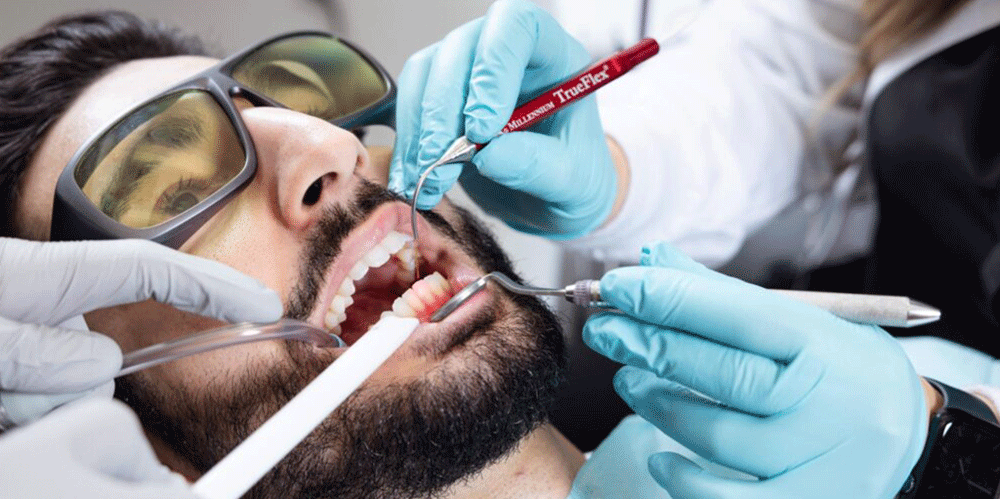
Periodontal disease examination involves evaluation of the gingiva for inflammation and the underlying attachment structures for the formation of pockets and bone loss. To diagnose gingivitis, your dentist will use a periodontal probe, a small, blunt device calibrated in millimeters, to assess the gingiva for color change and the gingival sulcus for bleeding. The periodontal probe is gently inserted between the tooth and gingiva until a slight opposition is felt.
Aside from redness, bleeding in response to gentle probing is also an indication of gingivitis.
The periodontal probe is also used to measure the periodontal pockets. If the probe can be inserted beneath the gingiva up to 3-4 mm or more, you have periodontal pockets that signify the destruction of the periodontal ligament and alveolar bone resorption.
Oral radiographs help to measure the extent of bone loss. If periodontal disease is progressive, the teeth usually get mobile, which is considered an additional indication of periodontal ligament and alveolar bone loss.
You may not be able to detect or diagnose periodontal disease by yourself as they are primarily painless and asymptomatic. Bleeding gums caused by tooth brushing is often the first symptom of gingivitis. The first indication of periodontitis, however, is the loosening of the teeth.
Asymptomatic gingiva can be misleading because there may be considerable loss of the attachment structures underneath. However, severe gingivitis does not necessarily mean that the underlying structures are destroyed.

Epidemiology
Studies performed by the national center for health statistics maintain that several factors influence the prevalence of periodontal disease: Loss of fewer teeth due to the use of fluoride, longer life expectancy, and changes in educational level and dental care.
The antiseptic properties of fluoride can decrease bacterial accumulation and chances of developing gingivitis. Likewise, antibiotics can decrease the prevalence and severity of periodontal diseases.
Thanks to recent advancements in dentistry, teeth are protected from cavities, and periodontal diseases are usually diagnosed in their early stages. This is of great significance as it has a direct effect on life expectancy.
People nowadays are aware of the importance of early periodontal disease detection. They are constantly reminded by the media or at schools to go for regular dental check-ups, at least once a year.
History and progression of periodontal disease
Long-term epidemiologic studies have reported that the severity of the periodontal disease increases with age. Periodontal disease will progress quickly if left untreated, leading to the eventual loss of teeth.
Gingivitis precedes periodontitis, therefore it’s safe to say that people with untreated moderate to advanced periodontal disease face progressive increases in pocket depth and loss of alveolar bone in one to ten years. The progression of periodontal disease is slow among those who initially show mild gingivitis and no periodontitis. However, the rate of bone loss will be more rapid among people older than 35.
Studies show that if you do not treat periodontal disease, it will eventually become episodic, causing tooth loss.
Cause
Accumulation of bacteria on the tooth’s surface and under the gingiva was initially believed to be the reason for periodontal diseases. However, the responsible bacteria were not determined. It was generally believed that all bacteria on the teeth could cause periodontal disease, and the number of bacteria had a direct effect on the development and severity of the disease.
We now know that periodontal disease is caused by specific bacteria in the periodontal pocket. However, how much of the periodontal tissue destruction is a direct after-effect of the bacteria and how much of it is caused by the body’s reaction to the bacteria still remain a mystery.
The bacteria present in the periodontal pocket may directly affect histolytic enzymes, endotoxins, exotoxins, and factors interfering with cell function. Collagenase and proteases released by bacteria in the periodontal pocket could also wreak havoc on the teeth. Bacteria may also interfere with the standard defense mechanisms of your body by deactivating specific antibodies or preventing their death. Bacteria in the periodontal pocket can kill human lymphocytes, platelets, or fibroblasts and induce bone destruction.
Aside from bacterial substances directly destroying the periodontal tissues, how your body reacts to such substances can be another reason for the destruction. In acute infections, the pathogenic manifestations of the disease may be caused directly by the bacteria through the invasion of the tissue and the production of toxic substances that lead to cell death and tissue necrosis.
The responses are often protective and do not contribute to the disease progression. They are immunopathologic processes resulting in the alteration of fibroblast function, the activity of macrophages releasing lytic enzymes, the activation of lymphocytes, the modulation of fibroblast growth, synthesis of collagen, and the stimulation of bone resorption.
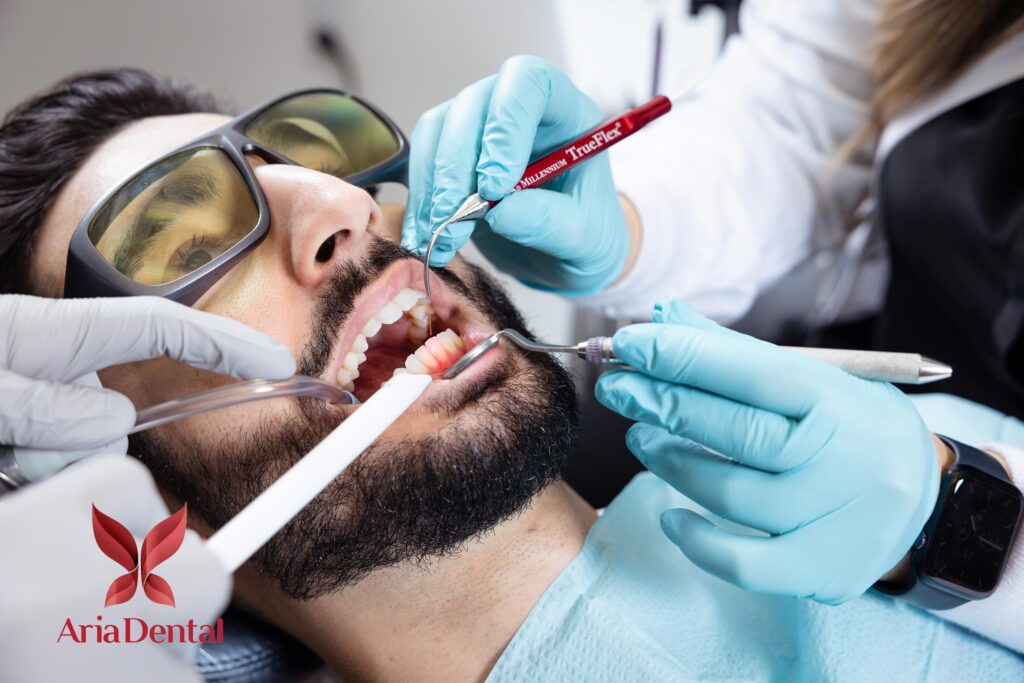
Periodontics
Periodontics is a branch of dentistry that focuses on the health of bones and tissues supporting your teeth, helping to prevent periodontal diseases and offering patients a personalized treatment plan to control the infection. Depending on the severity of the disease, various treatments are available, all requiring you to maintain proper dental care and follow a healthful lifestyle.
- Periodontal scaling and root planning
Scaling and root planning, also known as deep cleaning, is a unique non-surgical practice as the first line of defense against gum diseases. This approach involves utilizing an advanced ultrasonic scaler device and other special instruments to remove the plaque from your mouth.
During a procedure called periodontal debridement, accumulated plaque on the teeth can be removed to smooth out the root surface and provide a clean texture to help with easy reattachment of the gum tissue to the tooth.
- Gross debridement
If the patient has put off dental care, a regular teeth cleaning may no longer suffice. In that case, gross debridement, followed by a prophylaxis cleaning, is usually employed to thoroughly remove tartar and plaque from the teeth and gums.
- Periodontal maintenance therapy
If you have a history of gum disease, periodontal maintenance cleaning is recommended to ensure a lifetime of healthy teeth and gums. This technique employs a comprehensive examination and involves a complete cleaning to prevent gum disease.
X-rays and visual examination of the mouth are the first step, followed by the removal of the calculus along and under the gumline. Next, dental scaling tools are used for supragingival cleaning. Finally, any remaining bacteria is removed by gently smoothing the teeth.
- Oxygen / Ozone therapy
This therapy is a holistic approach to naturally reduce oral bacteria without the use of pharmaceutical drugs. This treatment has different applications: Ozonated water, ozonated oils, and applying oxygen/ozone directly into the infected gum pockets.
- Soft-tissue diode lasers
Dental diode lasers, sometimes called soft tissue lasers, are quite ideal for precisely cutting the gingiva and removing bacteria contributing to gum disease. This technique uses laser light to ensure the return of the periodontium to its healthy status.
- LANAP® laser therapy
PerioLase® LANAP, the first FDA-approved laser-assisted technique, is an invasive treatment used to target moderate to severe gum diseases. This modern technique removes the diseased tissues without damaging the healthy gum. LANAP requires no cut, stitch, or drill and is virtually painless. It is the only method proven to yield accurate periodontal regenerating results by killing the dangerous bacteria and stimulating your existing stem cells.
- Perio Trays®
The Perio Tray® is an improved periodontal treatment and an easy, non-invasive approach for eliminating the factors that cause gum disease, ultimately helping to restore your oral health.
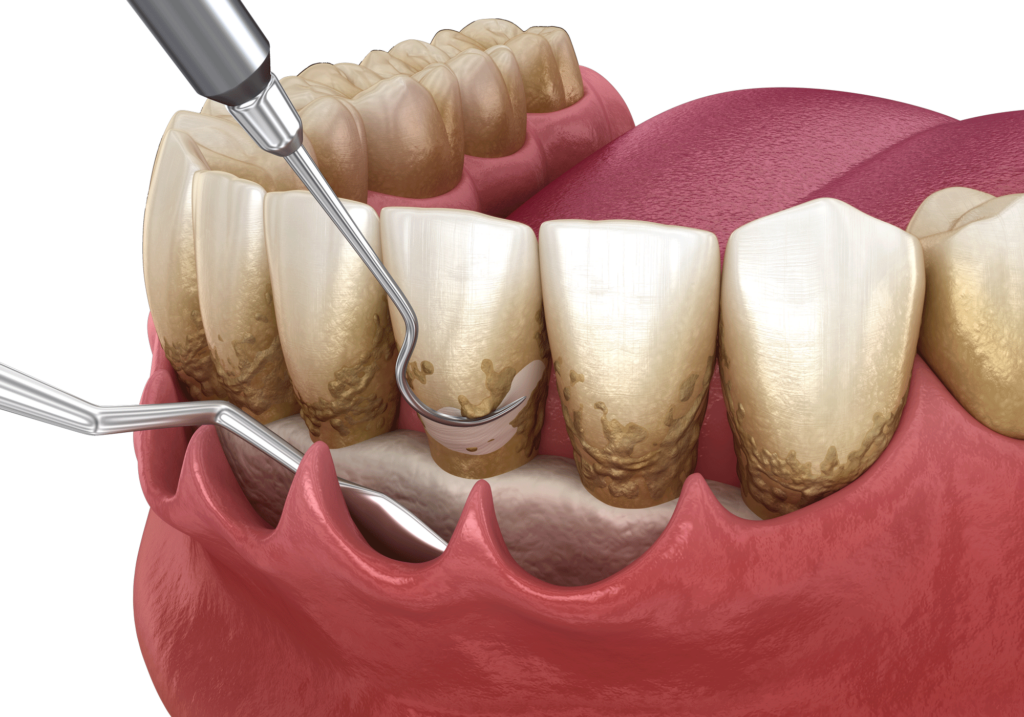
- Surgical periodontal treatment
Failing to promptly treat gingivitis and periodontitis, or any gum disease in general, could dramatically compromise your oral and overall health. Gum diseases may damage the bones and cause holes to develop in them.
When the damage to the tissues or the bone surrounding your teeth is too severe to be repaired through non-surgical treatments, periodontal surgery steps in to reshape deformations and remove pockets in the bones.
During this procedure a local anesthetic is applied before lifting the gum tissue away from the tooth’s surface to clean any plaque on the tooth. After thoroughly cleaning the roots, specific tools are used to reshape the damaged bones. A periodontal dressing will cover the target side in the end. Medications are generally prescribed following the surgery.
Aria Dental
Our attentive staff is prepared to offer the best solution for your gum conditions. Aria Dental dentists are accredited to perform any treatment for your gums to help you refresh your oral health.