A dental bridge can be a life-changing restoration, closing the gap left by one or more missing teeth, restoring your bite, and giving you back a confident smile. But like any dental prosthesis, a bridge requires ongoing vigilance. One of the most serious, and most commonly overlooked, complications is a dental bridge infection. When it goes undetected, an infection under or around a dental bridge can silently destroy the surrounding teeth, gum tissue, and bone, eventually leading to prosthesis failure and significant health consequences.
At Aria Dental Care in Orange County, Dr. Maryam Horiyat has spent decades helping patients understand, prevent, and treat dental bridge infections before they escalate. In this comprehensive guide, we’ll walk you through the key dental bridge infection symptoms, explain why they occur, and show you exactly what to do if you recognize any of them, so you can protect your oral health and your investment.
What Is a Dental Bridge Infection and Why Does It Happen?
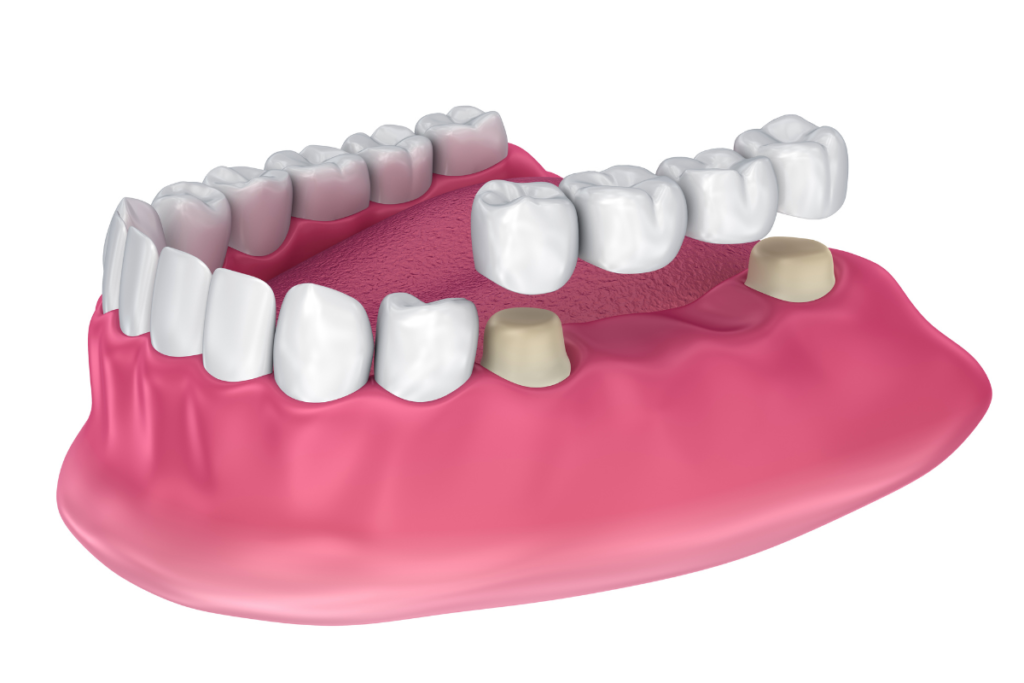
A dental bridge is a fixed dental prosthesis that spans the gap created by one or more missing teeth. It is anchored on either side by dental crowns placed over the adjacent natural teeth, called abutment teeth, or by dental implants. A pontic (the artificial tooth in the middle) fills the space where the missing tooth once was.
Unlike dental implants, a traditional tooth-supported bridge relies on the structural integrity of the neighboring natural teeth. This means those abutment teeth must be permanently altered, filed down to accommodate the crowns, and they carry the full functional load of the bridge. Over time, this creates an environment where bacteria can more easily accumulate, particularly at the margins where the crown meets the gum tissue and where the underside of the pontic sits above the gum.
According to the American Dental Association (ADA), dental bridges require meticulous hygiene maintenance specifically because of the difficulty in cleaning beneath the pontic. When oral hygiene is inadequate, or when the bridge fit is imperfect, bacteria colonize these hard-to-reach spaces, initiating the cascade of decay and infection that constitutes dental bridge infection.
The most common root causes include:
- Poor oral hygiene, Failure to floss beneath the bridge using a floss threader or water flosser allows plaque and bacteria to accumulate unchecked
- Ill-fitting bridge margins, Gaps or ledges at the crown-tooth junction provide bacterial entry points
- Pre-existing gum disease (periodontitis), Active gum disease dramatically accelerates infection risk under and around bridges
- High-sugar or high-carbohydrate diet, Feeds the bacteria responsible for decay beneath the bridge
- Tooth decay in the abutment teeth, If decay develops in the teeth supporting the bridge, infection can spread beneath the crowns and deep into the tooth structure
Understanding these causes is the first step. But recognizing the symptoms of dental bridge infection is what allows you to act before the damage becomes irreversible.
7 Critical Dental Bridge Infection Symptoms You Must Know
If you experience one or more of the following signs, do not delay, contact your holistic dentist for an urgent evaluation.
Symptom #1: Tooth Sensitivity or Hypersensitivity Near the Bridge
The very first signal of an underlying dental bridge problem is often tooth sensitivity, those sharp, electric-like sensations you feel when eating or drinking something hot, cold, or sweet. This hypersensitivity occurs at or near the site of your bridge and can catch you off guard during an otherwise ordinary meal.
Sensitivity signals that the enamel, and potentially the dentin beneath, of one or both abutment teeth has been compromised. This compromise most commonly happens because tooth decay has begun developing at the margins of the bridge crowns, where the restorative material meets the tooth surface. If decay is allowed to progress, it will eventually reach the nerve of the tooth, causing escalating pain and potentially leading to abscess formation.
Sensitivity can also arise if the cement holding the bridge in place has begun to wash out, a process that creates microscopic gaps where bacteria can freely enter. Even if you don’t experience any other dental bridge infection symptoms yet, persistent sensitivity near your bridge should prompt an immediate dental visit.
What distinguishes infection-related sensitivity from normal sensitivity:
- It is localized specifically to the bridge site, rather than widespread
- It lingers for more than a few seconds after the stimulus is removed
- It worsens progressively over days or weeks rather than improving
- It occurs spontaneously, without any hot, cold, or sweet trigger
- It is accompanied by other symptoms on this list
Symptom #2: Persistent or Worsening Pain Around the Bridge Site
While some degree of adjustment discomfort is normal immediately after a dental bridge is placed, pain that persists, returns, or worsens after the initial settling period is not normal. Ongoing or escalating pain around a dental bridge is one of the most telling dental bridge infection symptoms and should never be dismissed as “just part of having a bridge.”
Infection-related pain typically has a different character from ordinary soreness. It may present as a deep, throbbing ache that is difficult to pinpoint, a constant dull pressure across the jaw, or sharp pain triggered by biting down on the bridge. In more advanced cases, when infection has reached the pulp (nerve) of an abutment tooth, the pain can become severe, radiating into the jaw, cheek, temple, or ear.
This type of referred pain is commonly mistaken for a sinus issue, jaw problem, or tension headache, which is why many patients unknowingly delay getting the dental evaluation they need. The National Institutes of Health (NIH) has extensively documented the relationship between untreated dental infections and referred orofacial pain, reinforcing that any unexplained jaw or facial pain deserves proper dental screening.
Red flags that your bridge pain may indicate infection:
- Pain that began weeks or months after bridge placement rather than immediately
- Pain that wakes you at night
- Throbbing or pulsing sensations at the bridge site
- Pain that worsens with pressure or biting
- Pain that doesn’t respond to over-the-counter pain relievers
Symptom #3: Swelling, Redness, or Inflammation of the Surrounding Gum Tissue
Healthy gum tissue around a dental bridge should be firm, pink, and snug against the margins of the crowns. When infection sets in, the gum tissue responds with inflammation, becoming red, puffy, tender to the touch, and visibly swollen. This localized gum inflammation is one of the most reliable early dental bridge infection symptoms, and it’s one that patients can often see for themselves simply by looking in the mirror.
The swelling occurs because the immune system is actively fighting a bacterial infection at that site. As the body sends increased blood flow and immune cells to the area, the gum tissue becomes engorged and sensitive. Left untreated, this localized gingival inflammation can progress to periodontitis, a deeper infection involving the bone, which compromises the stability of the abutment teeth and puts the entire bridge at risk.
In some cases, the swelling may extend beyond the immediate gum tissue into the cheek or face. Facial swelling in the context of a dental bridge is a serious sign indicating that the infection has potentially spread beyond the localized gum tissue, possibly forming a dental abscess. This constitutes a dental emergency.
Signs that gum swelling is infection-related:
- Swelling persists for more than a few days without improving
- The gum tissue bleeds spontaneously or when lightly touched
- The affected gum looks noticeably different in color (dark red or purplish) compared to surrounding gum tissue
- Swelling is accompanied by warmth at the site or fever
- Swelling extends to the face, jaw, or neck, seek emergency care immediately
Symptom #4: Visible Pus or Discharge Around the Bridge Margins
If you notice any pus, discharge, or white/yellow fluid oozing from the gum tissue around your dental bridge, at the crown margins or beneath the pontic, this is one of the clearest and most serious dental bridge infection symptoms. Pus is the body’s direct response to a bacterial infection: a concentrated collection of dead bacteria, immune cells, and tissue debris.
The presence of pus indicates that the infection has progressed beyond early-stage gum inflammation. It suggests that bacteria have established a significant foothold in the periodontal pocket around one or both abutment teeth, and that the body’s immune response has not been sufficient to contain it. At this stage, professional treatment is non-negotiable. No amount of rinsing, home remedies, or over-the-counter products will resolve a purulent dental bridge infection.
You may notice pus when you apply gentle pressure to the gum near the bridge, during brushing or flossing, or even spontaneously throughout the day. It is often accompanied by a distinctly foul taste and persistent bad breath. If you observe any of these signs, contact Aria Dental Care without delay for an urgent appointment.
Symptom #5: Bad Breath or Persistent Bad Taste That Won’t Go Away
Chronic halitosis (bad breath) or a foul, metallic, or bitter taste in your mouth that refuses to clear up with brushing, flossing, or mouthwash is a highly significant, and frequently ignored, symptom of dental bridge infection. Many patients attribute ongoing bad breath to diet, dry mouth, or stomach issues. But when the odor or taste is localized to the area of the bridge, the cause is almost always bacterial.
The bacteria responsible for gum disease and periodontal infection produce volatile sulfur compounds (VSCs), the chemical byproducts that create the offensive smell characteristic of dental infections. These VSCs arise from the breakdown of proteins in the infected tissue, and because they emanate from beneath the bridge or within infected gum pockets, standard oral hygiene measures can’t eliminate them at their source.
A persistent foul taste, in particular, may indicate the presence of active pus in the gum tissue, even when the discharge isn’t immediately visible. From a holistic dental perspective, this symptom is viewed as a signal of systemic bacterial burden, an oral health issue that may have implications extending beyond just the bridge site.
When bad breath signals a dental bridge problem:
- The odor is localized and others have mentioned it to you
- Brushing, flossing, and mouthwash provide only very temporary relief
- The taste in your mouth has changed since your bridge was placed or adjusted
- The bad breath is accompanied by any other dental bridge infection symptoms on this list
- You can taste or smell something unusual when you press your tongue or finger near the bridge
Symptom #6: Loosening, Shifting, or Ill-Fitting Feel of the Bridge
A well-fitted dental bridge should feel completely stable, immovable, comfortable, and completely natural in your bite. If your bridge begins to feel loose, wobbly, or “off” in any way, or if your bite feels uneven when the bridge was previously comfortable, these changes may indicate a serious problem developing beneath the restoration.
A loose dental bridge most commonly occurs when the cement bond between the crown and the abutment tooth has been compromised. This can happen due to bacterial infiltration at the margin, cement washout, or structural changes in the underlying tooth. When the bond fails, bacteria gain direct access to the prepared tooth structure underneath the crown, dramatically accelerating the risk of decay and deep infection.
Alternatively, if bone loss has occurred due to periodontal infection around an implant-supported bridge, the implant anchor may become destabilized, causing movement of the entire prosthesis. In either scenario, a bridge that shifts or feels different from how it once did should be examined by a dentist within days, not weeks.
Symptom #7: Fever, Swollen Lymph Nodes, or General Illness
When a dental bridge infection progresses beyond the localized oral structures, the body begins to show systemic signs of fighting infection. A low-grade or high fever, swollen lymph nodes in the neck or under the jaw, general fatigue, or a feeling of being unwell alongside dental symptoms is an extremely serious warning combination that demands emergency dental care without delay.
These systemic symptoms suggest that the infection may have spread to deeper tissues of the jaw, neck, or, in the most severe cases, the bloodstream. Dental sepsis, while relatively rare, is a life-threatening condition that has been documented as a consequence of untreated dental infection. Research published in MedlinePlus (National Library of Medicine) and other high-authority health databases consistently highlights the systemic health consequences of unmanaged oral infections, including their link to cardiovascular disease, diabetes complications, and respiratory illness.
If you experience fever, difficulty swallowing, significant facial or neck swelling, or rapidly worsening symptoms alongside any of the dental bridge infection symptoms listed above, go to an emergency room or call emergency services immediately.
Why Dental Bridge Infections Are More Common Than Most People Realize
Many patients are surprised to learn how frequently dental bridge infections occur. The prosthesis design itself creates inherent hygiene challenges that, when combined with natural factors like gum tissue changes and dietary habits, make consistent bacterial management difficult.
The Pontic Problem
The pontic, the false tooth at the center of a traditional dental bridge, rests just above the gum tissue rather than being anchored within it. This creates a space beneath the pontic that traps food particles, plaque, and bacteria. Unless patients use specialized hygiene tools (floss threaders, interdental brushes, or water flossers) to clean beneath the pontic every single day, this space becomes a breeding ground for the bacteria responsible for gum disease and bridge-related infection.
Abutment Tooth Vulnerability
Because the abutment teeth supporting the bridge must be permanently altered, ground down and capped with crowns, they become permanently reliant on the integrity of that restoration. The margin where the crown ends and the natural tooth structure begins is a perpetual vulnerability. Over years of normal use, these margins can develop microscopic gaps that allow bacteria to infiltrate the tooth structure beneath the crown, completely out of reach of any cleaning tool and invisible without dental X-rays.
The Holistic Perspective on Bridge Infections
From a holistic and biological dentistry standpoint, the risk of dental bridge infection doesn’t exist in isolation. At Aria Dental Care, Dr. Maryam Horiyat evaluates the full picture, including systemic health, nutritional status, immune function, and the biocompatibility of the materials used in the restoration. Patients with conditions that suppress immune function (including uncontrolled diabetes, autoimmune disorders, or chronic stress), as well as those who smoke, are at significantly elevated risk for developing bridge-related infections.
This whole-body perspective is what sets a truly holistic approach to dental care apart. Rather than simply treating the visible symptoms, Dr. Horiyat investigates and addresses the underlying factors that make a patient susceptible to oral infection in the first place.
How Are Dental Bridge Infections Diagnosed?
When you present at Aria Dental Care with potential dental bridge infection symptoms, Dr. Horiyat conducts a comprehensive clinical evaluation that goes far beyond a visual inspection. This typically includes:
- Digital periodontal probing to measure pocket depth around the abutment teeth, a direct clinical indicator of gum and bone infection
- Digital X-rays to reveal decay beneath the crowns, bone loss, or abscess formation that is invisible to the naked eye
- 3D Cone Beam CT (CBCT) scanning for complex cases requiring a full three-dimensional view of the bone, roots, and surrounding anatomy
- Assessment of bridge stability and margin integrity, checking for looseness, open margins, or cement failure
- Evaluation of the opposing bite to identify excessive pressure contributing to bridge stress
This diagnostic thoroughness is critical because the early stages of dental bridge decay and infection are often completely invisible without radiographic evaluation. Many patients arrive without pain or obvious symptoms, yet X-rays reveal significant decay developing beneath the crowns. This is precisely why regular six-month monitoring appointments are not optional when you have a dental bridge, they are your most powerful tool for catching problems before they become catastrophic.
Treatment Options for Dental Bridge Infection
The appropriate treatment depends entirely on how advanced the infection has become at the time of diagnosis.
Early-Stage Treatment: Infection Confined to Gum Tissue
When dental bridge infection symptoms are caught early, before decay has penetrated the abutment tooth pulp or before significant bone loss has occurred, treatment is more conservative and highly effective. Approaches may include:
- Professional deep cleaning (scaling and root planing) to remove bacterial deposits from the root surfaces beneath the gum tissue
- Laser-assisted periodontal therapy to decontaminate infected pockets with minimal discomfort and excellent precision
- Antibiotic therapy, either systemic (oral) or localized (antibiotic gel placed directly into the infected periodontal pocket)
- Bridge removal, thorough cleaning, and recementation if the infection is related to cement washout or marginal leakage
- Rigorous enhanced home care protocol including daily use of a water flosser, antimicrobial rinse, and floss threader
Intermediate Treatment: Decay in the Abutment Teeth
When tooth decay has developed beneath the bridge crowns but has not yet reached the dental pulp, treatment may involve bridge removal, excavation and filling of the cavity, and fabrication of a new bridge with properly sealed margins. If the decay is extensive, additional preparatory work, including potential root canal treatment, may be required before a new restoration can be placed.
Advanced Treatment: Pulp Involvement, Abscess, or Bone Loss
When infection has reached the nerve of an abutment tooth, root canal therapy may be necessary to remove the infected tissue and save the tooth before the bridge is replaced. If an abscess has formed, it must be drained and the infection cleared systemically with antibiotics before definitive restorative work can proceed.
In cases where the abutment teeth have been so severely damaged by decay or infection that they cannot be saved, extraction followed by implant placement may represent the healthiest, most durable long-term solution. At Aria Dental Care, this transition is handled with meticulous attention to biocompatibility, using zirconia implants and biocompatible restorative materials to give patients the cleanest, most biologically sound outcome possible.
How to Prevent Dental Bridge Infection: Holistic Best Practices
The best treatment for dental bridge infection is prevention. Here is what Dr. Horiyat recommends to every bridge patient:
- Master the art of cleaning under your bridge: Use a floss threader to pass dental floss beneath the pontic every single day. A water flosser is an excellent complement for flushing out debris from beneath and around all bridge margins.
- Use an antibacterial rinse: An antimicrobial mouthwash used consistently helps reduce the bacterial load throughout the oral cavity, including in the hard-to-reach spaces beneath the bridge.
- Never miss your maintenance appointments: Schedule professional dental check-ups and cleanings every six months, or more frequently if your dentist recommends it. These appointments include X-rays that can detect decay beneath the bridge before it becomes symptomatic.
- Eliminate or reduce sugar and processed carbohydrates: These substances directly fuel the bacteria that cause decay and gum disease beneath bridges.
- Address systemic health factors proactively: Work with your physician to manage conditions like diabetes, nutritional deficiencies, or immune-suppressing medications that increase infection risk.
- Quit smoking: Smoking impairs gum tissue healing, suppresses immune function at the gum level, and dramatically accelerates the development of periodontal infection.
- Report any new symptoms promptly: The moment you notice sensitivity, pain, swelling, or any other dental bridge infection symptom, call your dentist. Early intervention is always simpler, less expensive, and more successful than delayed treatment.
Is a Dental Implant a Better Long-Term Alternative to a Bridge?
This is a question Dr. Horiyat is frequently asked, and it’s an important one. Traditional tooth-supported dental bridges, while effective restorations, carry inherent limitations: they require alteration of healthy abutment teeth, create cleaning challenges, and, as this article has documented, carry a meaningful risk of infection over time.
Dental implants, by contrast, are independent, self-anchored restorations that require no modification of adjacent teeth, are easier to clean with standard hygiene tools, and, particularly when made from zirconia, carry a dramatically lower risk of infection or biological complication. Zirconia implants, the specialty of Aria Dental Care, possess a smooth, bacteria-resistant ceramic surface that is far less hospitable to plaque accumulation than both titanium implants and the crown margins of traditional bridges.
For patients who are experiencing repeated bridge infections, whose abutment teeth have been compromised by decay, or who are considering tooth replacement for the first time, the conversation about dental implants as a more durable and biologically sound long-term solution is absolutely worth having with your holistic dentist.
Trusted External Resources on Dental Bridge Health
For further reading from high-authority dental health sources, we recommend:
- American Dental Association (ADA), Bridges: Oral Health Topics
- National Institutes of Health (NIH / NCBI), Orofacial Pain and Dental Infection Research
- MedlinePlus (National Library of Medicine), Dental Health Overview
Frequently Asked Questions About Dental Bridge Infection Symptoms
Q1: How do I know if my dental bridge is infected or if I’m just experiencing normal sensitivity?
Normal sensitivity immediately after a bridge is placed, particularly in the first 1–2 weeks, is common and typically resolves as the gum tissue and abutment teeth adjust. Infection-related sensitivity, on the other hand, tends to develop or worsen over time rather than improve, persists long after the bridge was placed, and is often accompanied by at least one other dental bridge infection symptom such as swelling, bleeding gums, or a foul taste. The most reliable way to distinguish the two is a prompt dental evaluation that includes X-rays, which can reveal decay beneath the bridge that the naked eye cannot.
Q2: Can a dental bridge infection spread to other teeth or the rest of the body?
Yes, and this is one of the most important reasons to take dental bridge infection symptoms seriously from the outset. An untreated bacterial infection in the gum tissue around a bridge can spread laterally to adjacent teeth, causing decay and periodontal disease throughout the surrounding dentition. In more advanced or rapidly progressing cases, the infection can migrate into deeper jaw structures, the lymph nodes, or, in severe cases, the bloodstream, a life-threatening condition known as sepsis. Dental infections have also been linked by extensive research to systemic conditions including cardiovascular disease, poorly controlled diabetes, and respiratory infections.
Q3: What happens if I ignore dental bridge infection symptoms and don’t seek treatment?
Ignoring dental bridge infection symptoms allows the bacterial infection to progress unchecked. Tooth decay beneath the crowns will advance toward the pulp of the abutment teeth, ultimately causing pulp death, abscess formation, and potentially the loss of those teeth entirely. Gum disease will progress, causing bone loss around the abutment teeth and potentially destabilizing the bridge. The bridge itself will eventually fail, requiring removal. What could have been resolved with a cleaning, antibiotic, or simple bridge recementation at the earliest stage may ultimately require extractions, bone grafting, and complete arch reconstruction if left untreated.
Q4: How long do dental bridges typically last, and does infection shorten their lifespan?
With excellent oral hygiene and regular professional maintenance, a dental bridge can last 10–15 years or longer. However, a dental bridge infection, even when successfully treated, can significantly compromise the structural integrity of the abutment teeth supporting the bridge, shortening its effective lifespan. Repeated infections, or an infection that results in significant decay or bone loss in the abutment teeth, often necessitate premature bridge replacement or a transition to implant-based restoration. The single most impactful thing a bridge patient can do to maximize longevity is maintain daily cleaning beneath the bridge and never skip professional maintenance appointments.
Q5: Should I replace my dental bridge with a dental implant if I keep getting infections?
This is a conversation worth having with your holistic dentist, and the answer depends on the condition of your abutment teeth and your overall oral health. If you have experienced one dental bridge infection that was caught and treated early, a replacement bridge with improved margins and enhanced hygiene protocols may be fully adequate. However, if you have experienced recurrent infections, if your abutment teeth have been substantially weakened by decay, or if you are seeking a longer-term solution with a lower infection risk, a dental implant is likely the superior biological choice. At Aria Dental Care, Dr. Horiyat will conduct a comprehensive evaluation and discuss all options transparently, including zirconia implants, which offer exceptional biocompatibility and dramatically reduced bacterial adhesion compared to both bridges and titanium implants.
Conclusion: Recognizing Dental Bridge Infection Symptoms Could Save Your Smile
A dental bridge is a meaningful investment in your oral function and quality of life, and like any investment, it deserves vigilant protection. Dental bridge infections are preventable, and when they do occur, they are highly treatable when caught early. The key is knowing what to look for.
To summarize the 7 dental bridge infection symptoms you should never overlook:
- Tooth sensitivity or hypersensitivity near the bridge site
- Persistent or worsening pain around the bridge
- Swelling, redness, or inflammation of the surrounding gum tissue
- Visible pus or discharge at the bridge margins
- Chronic bad breath or bad taste that persists despite oral hygiene
- Bridge looseness or a shifting bite
- Fever, swollen lymph nodes, or systemic illness alongside dental symptoms
At Aria Dental Care, we are proud to serve Orange County as the region’s #1 holistic, biological, and cosmetic dental office. Under the expert and compassionate leadership of Dr. Maryam Horiyat, who brings decades of specialized training and thousands of successfully treated patients to every case, we deliver the highest standard of biocompatible, patient-centered dental care available in Southern California.
Whether you are concerned about your existing dental bridge, experiencing any of the symptoms described in this article, or are exploring whether an implant might be a healthier long-term option for you, our team is here to help. We invite you to schedule a consultation with Dr. Horiyat and experience the Aria Dental difference.
At Aria Dental Care, your health is not just our mission, it is our highest honor.
Schedule Your Consultation Today Aria Dental Care | Orange County, CA ariadentalcare.com