Dental implants are one of the most transformative solutions in modern dentistry. They restore your smile, preserve jawbone integrity, and function just like natural teeth. But what happens when something goes wrong after placement? A dental implant infection, though not common, is a serious complication that demands prompt attention. Recognizing the early warning signs can mean the difference between saving your implant and losing it entirely.
At Aria Dental Care in Orange County, Dr. Maryam Horiyat brings decades of specialized holistic and biological dental expertise to every patient she treats. In this comprehensive guide, we’ll walk you through the five most important signs of a dental implant infection, explain what causes them, discuss how they’re diagnosed and treated, and share how a holistic approach to implant dentistry can dramatically reduce your risk.
What Is a Dental Implant Infection, and How Common Is It?
A dental implant infection occurs when bacteria colonize the tissue or bone surrounding an implant, triggering inflammation and potential structural damage. The most clinically recognized form is called peri-implantitis, a progressive condition involving inflammation of the soft and hard tissues around the implant site that, if left untreated, leads to bone loss and eventual implant failure.
Research published by the National Institutes of Health (NIH) indicates that between 4% and 10% of patients with traditional titanium dental implants may develop some form of peri-implant infection over their lifetime. The good news? Zirconia implants, the metal-free alternative that Aria Dental specializes in, show infection rates of less than 1%, thanks to their smooth, bacteria-resistant ceramic surface.
Understanding the difference between normal post-surgical discomfort and the early signs of a dental implant infection is essential. Some soreness, minor swelling, and brief sensitivity following implant placement are entirely expected as part of the healing process. These symptoms should resolve within a few days. When they persist, worsen, or are accompanied by other alarming symptoms, that’s when it’s time to take action.
5 Key Signs of a Dental Implant Infection You Must Watch For
If you recognize any of these warning signs in yourself or a loved one, contact your implant dentist immediately.
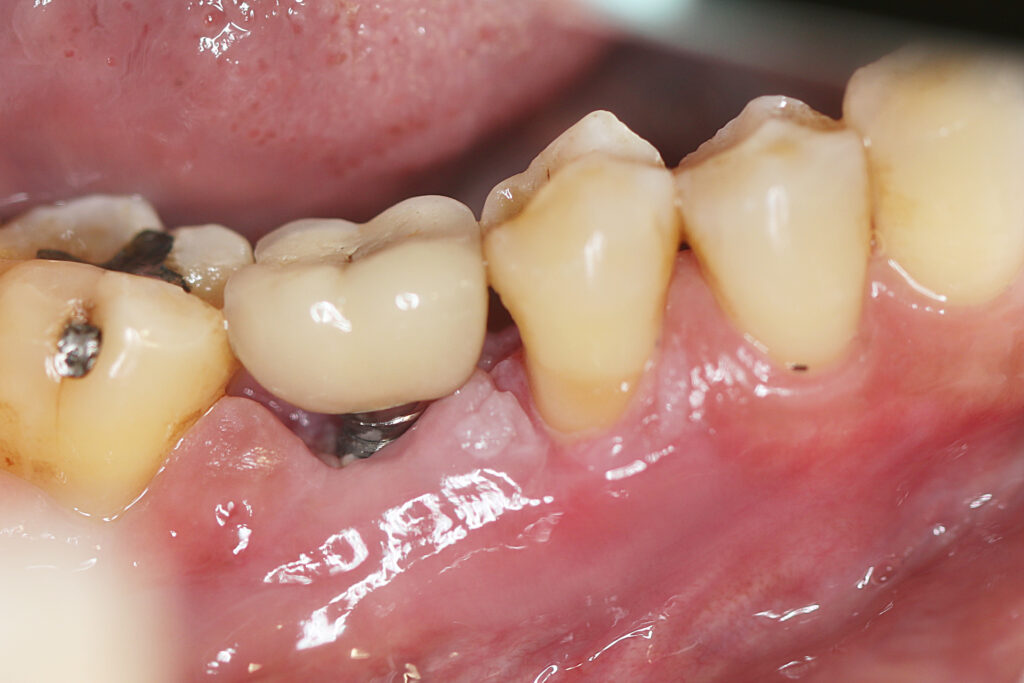
Sign #1: Persistent or Worsening Swelling and Redness Around the Implant Site
Swelling is a natural part of the body’s healing response to surgery. In a healthy recovery, peri-implant swelling peaks within 48–72 hours and gradually diminishes. When swelling persists beyond the first week, continues to worsen, or is accompanied by warmth and redness, it becomes a red flag for peri-implant infection.
Bacterial accumulation on the gum tissue and around the implant post is the primary driver of this inflammatory response. The bacteria trigger an immune reaction that causes the characteristic redness and swelling associated with peri-implant mucositis, the earlier, more reversible stage of dental implant infection. Catching the infection at this stage dramatically improves outcomes.
What to watch for:
- Gum swelling that does not resolve after the first 5–7 days post-surgery
- Redness that extends beyond the immediate implant site
- A feeling of heat or throbbing around the implant area
- Visible pus or discharge, a sign the infection has advanced
- Accompanying fever, which may indicate systemic spread
If any of these symptoms appear alongside fever or a foul taste in your mouth, do not wait for your next scheduled appointment. Contact Aria Dental Care immediately for an urgent evaluation.
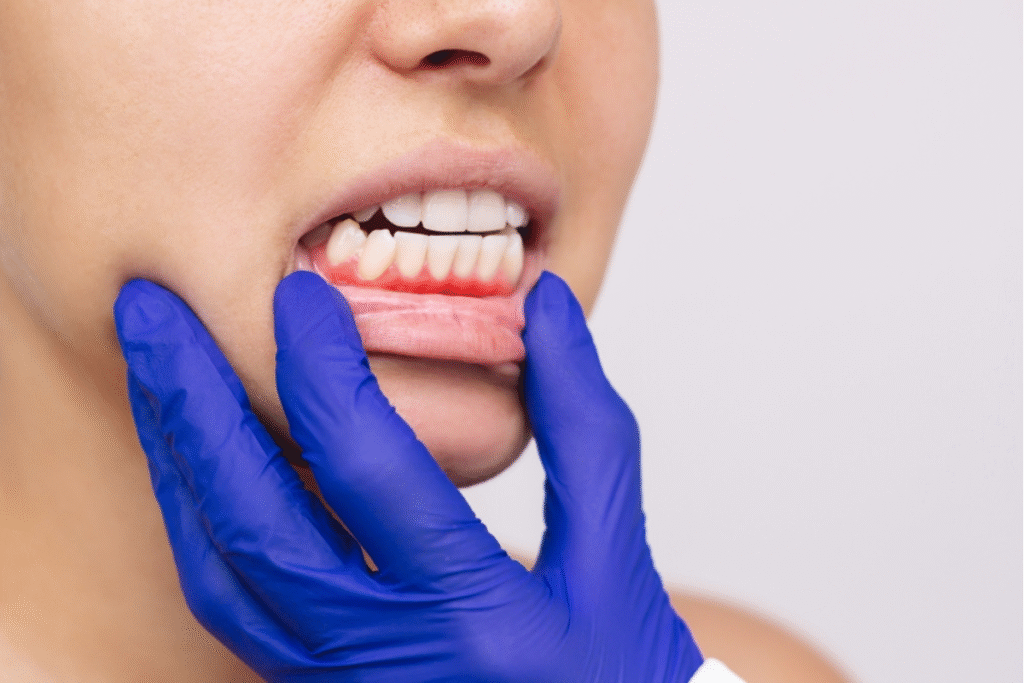
Sign #2: Unexplained or Prolonged Bleeding at the Implant Site
A small amount of bleeding in the first day or two following implant surgery is completely normal. Your gum tissue has just been sutured after a surgical procedure, some seepage is expected. However, ongoing or spontaneous bleeding, especially when it occurs days or weeks after surgery, or with routine activities like brushing and flossing, is not.
Abnormal bleeding from a dental implant site is frequently a sign of active gum infection. The inflamed, infected gum tissue becomes fragile and highly vascular, making it prone to bleeding at the slightest stimulus. When bleeding occurs spontaneously, without any brushing, flossing, or external pressure, it indicates that the infection may already be progressing into the deeper peri-implant structures.
Signs that bleeding is infection-related:
- Bleeding that starts or worsens after the initial 48-hour post-surgical period
- Blood visible during or after gentle brushing near the implant
- Spontaneous bleeding with no clear cause
- Bleeding combined with swelling and a bad taste in the mouth
- Pus-tinged discharge mixed with blood
Note: Certain medications, blood thinners, for example, can prolong bleeding for unrelated reasons. Always disclose your full medication history to your implant dentist, and still report any unexpected post-surgical bleeding promptly.
Sign #3: Persistent Bad Taste or Bad Breath That Won’t Go Away
Halitosis (bad breath) and an unusual taste in your mouth that refuses to resolve with brushing, mouthwash, or dental floss are among the most telling, and often underestimated, signs of a dental implant infection. Many patients initially dismiss this symptom, attributing it to diet or medication. But when it persists specifically in the area of the implant, it typically indicates bacterial activity beneath the gumline.
Bacteria involved in peri-implantitis and other forms of implant-related infection produce volatile sulfur compounds (VSCs), the same compounds responsible for the offensive odor associated with periodontal disease. These compounds are difficult to eliminate with surface oral hygiene alone because their source lies in the infected pockets of tissue surrounding the implant.
A foul metallic or bitter taste that doesn’t improve after thorough oral hygiene may also indicate the presence of pus in the gum tissue, a serious sign that requires professional evaluation without delay. In the context of a holistic dental practice, this symptom is viewed not just as a local oral health issue but as a potential signal of broader systemic inflammation that warrants comprehensive evaluation.
Sign #4: Pain or Discomfort That Persists or Escalates Over Time
Mild to moderate pain in the days following your dental implant procedure is expected. Most patients manage it comfortably with over-the-counter analgesics and find that it improves significantly within 3–5 days. What should raise immediate concern is pain that worsens after the initial healing period, or pain that returns after it seemed to be resolving.
A dental implant infection places significant pressure on the surrounding bone and soft tissue as the inflammatory process intensifies. This pressure manifests as deep, persistent, or throbbing pain that is distinctly different from the expected dull soreness of post-surgical healing. In some cases, patients describe it as similar to a toothache, an aching, pressure-filled sensation that radiates beyond the implant site into the jaw, cheek, or ear.
Pain patterns that suggest infection:
- Pain that worsens rather than improves after the first few post-surgical days
- Throbbing or pulsing pain at the implant site
- Pain that spreads to the jaw, adjacent teeth, or ear
- Discomfort when chewing or biting down on the implant
- Pain that recurs weeks or months after initially resolving
Dr. Horiyat’s clinical guideline: If your pain has not substantially improved within five days of surgery, or if pain returns after appearing to resolve, call your dentist immediately. Early intervention is always more effective, and less invasive, than treating an advanced infection.
Sign #5: Implant Looseness or Noticeable Movement
A successfully placed dental implant should feel exactly like a natural tooth, firmly anchored, immovable, and completely stable. If you notice any shifting, rocking, or looseness in your implant at any point, treat it as an urgent warning sign and contact your dentist immediately. Implant mobility is a serious late-stage indicator that something has gone significantly wrong.
Dental implant stability depends on a process called osseointegration, the direct structural bond between the implant post and the surrounding jawbone. When a dental implant infection advances to peri-implantitis, it causes progressive bone loss around the implant. As the supporting bone erodes, the implant loses its anchor and begins to move. At this stage, implant failure may be unavoidable without immediate aggressive intervention.
This is why Dr. Horiyat strongly emphasizes routine six-month checkups following implant placement. Bone loss can be identified on X-rays before it becomes symptomatic, allowing treatment to begin before the implant is compromised. During these visits, your dentist will also probe the tissue around the implant to measure pocket depth, a key clinical indicator of peri-implant health.
What Causes Dental Implant Infections? Understanding the Risk Factors
Knowledge is your first line of defense. Understanding the underlying causes and risk factors for implant-site infection empowers you to make proactive decisions about your dental and overall health.
Bacterial Contamination and Poor Oral Hygiene
The most common cause of peri-implant infection is the same culprit behind gum disease: bacterial plaque. When plaque is not adequately removed through regular brushing and flossing, it accumulates around the implant, irritates the surrounding gum tissue, and provides a breeding ground for the pathogenic bacteria responsible for peri-implantitis. Patients who had pre-existing periodontal (gum) disease before receiving their implant are at significantly higher risk.
Systemic Health Conditions and Immune Function
Conditions that compromise immune function or impair healing, including uncontrolled diabetes, autoimmune disorders, and certain medications like corticosteroids or immunosuppressants, increase the likelihood of dental implant complications, including infection. The body’s ability to mount an appropriate immune response around the implant site is critical to both preventing and clearing infection.
Smoking and Tobacco Use
Smoking is one of the most significant modifiable risk factors for dental implant failure and infection. Tobacco use restricts blood flow to the gum tissue, impairs the delivery of immune cells to the implant site, and dramatically slows the healing process. Smokers are considerably more likely to develop peri-implantitis and have lower implant success rates overall. Patients who smoke are strongly encouraged to quit before undergoing the implant procedure.
Implant Material: Titanium vs. Zirconia and Bacterial Adhesion
From a holistic and biological dentistry perspective, implant material matters enormously. Traditional titanium implants, while widely used and generally effective, have a rougher microscopic surface that makes them more prone to bacterial adhesion and plaque accumulation. Over time, titanium can also corrode in the moist oral environment, releasing metal ions into surrounding gum and bone tissue, which may trigger chronic inflammation, immune reactions, and hypersensitivity.
Zirconia implants, by contrast, possess a smooth, non-porous surface that is significantly less hospitable to bacterial colonization. They are fully metal-free, biologically inert, and have been shown to support excellent osseointegration with minimal inflammatory response. This is why, at Aria Dental Care, Dr. Horiyat recommends and places zirconia implants as the biological gold standard for patients seeking the healthiest possible outcome.
How Is a Dental Implant Infection Diagnosed and Treated?
If you present at Aria Dental Care with signs of a peri-implant infection, Dr. Horiyat will conduct a thorough clinical examination that includes probing the peri-implant pocket depth, evaluating the gum tissue for inflammation and suppuration (pus), and taking digital X-rays or a 3D Cone Beam CT scan to assess the extent of any bone loss.
Non-Surgical Treatment Approaches
When a dental implant infection is caught early, particularly at the stage of peri-implant mucositis (gum-level inflammation without significant bone loss), non-surgical treatments are often highly effective. These may include:
- Professional cleaning of the implant surface (mechanical debridement)
- Laser-assisted decontamination of the pocket
- Targeted antibiotic therapy
- Enhanced home care protocols using antibacterial rinses such as chlorhexidine
At Aria Dental, our approach to treating peri-implant infection is guided by holistic and biological principles. We use biocompatible treatment materials, minimize unnecessary antibiotic exposure where possible, and evaluate the full-body context of each patient’s health to address underlying contributing factors, not just surface symptoms.
Surgical Intervention for Advanced Peri-Implantitis
When peri-implantitis has progressed to include significant bone loss, surgical intervention is typically required. This may involve:
- Flap surgery to directly access and clean the implant surface
- Bone grafting to regenerate lost jawbone structure
- Implant surface decontamination using specialized instruments or laser energy
In cases where the infection has rendered the implant non-salvageable, implant removal followed by a healing and regeneration period, and ultimately replacement with a zirconia implant, may be the best path forward.
How to Prevent Dental Implant Infection: A Holistic Approach
Prevention is always superior to treatment, and at Aria Dental Care, prevention is built into every stage of the implant process. Here are the most important steps you can take to protect your implant and your oral health:
- Maintain impeccable oral hygiene: Brush at least twice daily, floss once daily, and use an antimicrobial or saline rinse, particularly in the early weeks after placement.
- Attend all follow-up appointments: Your six-month check-ups are not optional when you have implants. These visits allow your dentist to detect early signs of peri-implant disease before they progress.
- Address systemic health proactively: Work with your healthcare team to manage conditions like diabetes, autoimmune disease, or nutritional deficiencies that may compromise your healing capacity.
- Quit smoking: The single most impactful lifestyle change you can make for implant longevity.
- Choose biocompatible implant materials: If you have not yet received your implant, discuss zirconia as a lower-infection-risk, metal-free alternative with your holistic dentist.
- Report symptoms early: Don’t wait to see if things “clear up on their own.” If you notice any of the five warning signs described in this article, contact your dentist the same day.
Why Choose Aria Dental Care for Your Implant Health?
Dr. Maryam Horiyat is one of the most comprehensively trained holistic, biological, and cosmetic implant dentists in Southern California. Board-certified and accredited by multiple prestigious associations, including the International Academy of Oral Medicine and Toxicology (IAOMT) and the Certified Integrative Advisor in Biological Dentistry and Medicine (CIABDM), she brings a uniquely whole-body perspective to every implant case.
At Aria Dental Care, we don’t just treat teeth, we treat people. Our mission is to provide the highest quality, most biocompatible, and most health-conscious dental experience available in Orange County. That means using the latest 3D imaging technology to plan implants with precision, selecting the safest materials, and partnering with our patients in their long-term health journey.
Whether you’re experiencing symptoms of a possible dental implant infection, considering your first implant, or exploring healthier alternatives to conventional titanium implants, our team is here to guide you with compassion, expertise, and integrity.
Trusted External Resources on Dental Implant Health
For further reading from high-authority sources, we recommend:
- National Institutes of Health (NIH), Peri-implant diseases and conditions: A systematic review
- American Academy of Periodontology (AAP), Peri-Implant Diseases: Patient Education
- MedlinePlus (National Library of Medicine), Dental Health Overview
Frequently Asked Questions About Dental Implant Infection
Q1: How do I know if my dental implant is infected or just healing normally?
Normal healing after dental implant surgery typically involves mild swelling, tenderness, and some minor bleeding that resolves within 3–5 days. A dental implant infection, on the other hand, presents with symptoms that persist beyond this window, worsen over time, or include signs like pus, a persistent foul taste, fever, or an implant that feels loose. A general rule: if your symptoms are improving day by day, that’s healing. If they’re staying the same or getting worse after a week, call your dentist.
Q2: Can a dental implant infection heal on its own without treatment?
No, a dental implant infection will not resolve without professional treatment. Unlike a minor cut or bruise, the bacteria involved in peri-implantitis are pathogenic and self-sustaining in the biofilm around the implant surface. Without clinical debridement and appropriate treatment, the infection will progress, causing increasing bone loss and ultimately threatening the survival of your implant. Do not attempt to treat a suspected dental implant infection with home remedies alone.
Q3: How long after getting a dental implant can an infection develop?
Infections can develop at any point in the implant’s lifespan, not just in the initial healing period. Early-stage infections (peri-implant mucositis) can develop within the first weeks to months following placement. However, peri-implantitis, the more advanced form involving bone loss, can emerge years or even a decade after the implant was placed. This is precisely why lifelong maintenance appointments and routine monitoring are essential, not optional.
Q4: What antibiotics are used to treat a dental implant infection?
The antibiotic prescribed will depend on the severity and type of infection, as well as the patient’s medical history and any known drug sensitivities. Amoxicillin, metronidazole, or a combination of both are commonly used for peri-implant infections. However, antibiotics are typically used as an adjunct to, not a replacement for, mechanical cleaning and decontamination of the implant site. At Aria Dental Care, Dr. Horiyat takes a holistic and targeted approach to antibiotic use, prescribing only when clinically necessary to protect your broader microbiome health.
Q5: Can an infected dental implant be saved, or does it need to be removed?
Whether an infected implant can be saved depends largely on how quickly treatment is initiated and how far the infection has progressed. In the early stages (peri-implant mucositis), the infection is fully reversible and the implant can be preserved with conservative treatment. In moderate cases of peri-implantitis with limited bone loss, surgical intervention combined with bone regeneration may still save the implant. In severe cases with extensive bone destruction, implant removal may unfortunately be the only viable option, which is why early detection is so critical.
Conclusion: Don’t Ignore the Signs, Your Implant Health Matters
A dental implant is a significant investment in your long-term health, quality of life, and confidence. Protecting that investment means staying informed, practicing excellent oral hygiene, attending regular follow-up appointments, and, most importantly, acting quickly if any signs of dental implant infection appear.
To recap the five warning signs you should never ignore:
- Persistent or worsening swelling and redness around the implant
- Unexplained or prolonged bleeding at the implant site
- Bad taste or bad breath that won’t resolve with oral hygiene
- Pain or discomfort that persists or escalates over time
- Implant looseness or noticeable movement
At Aria Dental Care, we are proud to be Orange County’s #1 ranked holistic, biological, and cosmetic dental office. Under the expert leadership of Dr. Maryam Horiyat, we combine cutting-edge technology with deeply compassionate, whole-body care. If you have concerns about your dental implant, are experiencing any of the symptoms discussed in this article, or are considering implant treatment for the first time, we warmly invite you to schedule a consultation with our team.
Your health, oral and systemic, is our highest priority. Because at Aria Dental, we don’t just believe in beautiful smiles. We believe in healthy lives.
Schedule Your Consultation TodayAria Dental Care | Orange County, CA ariadentalcare.com